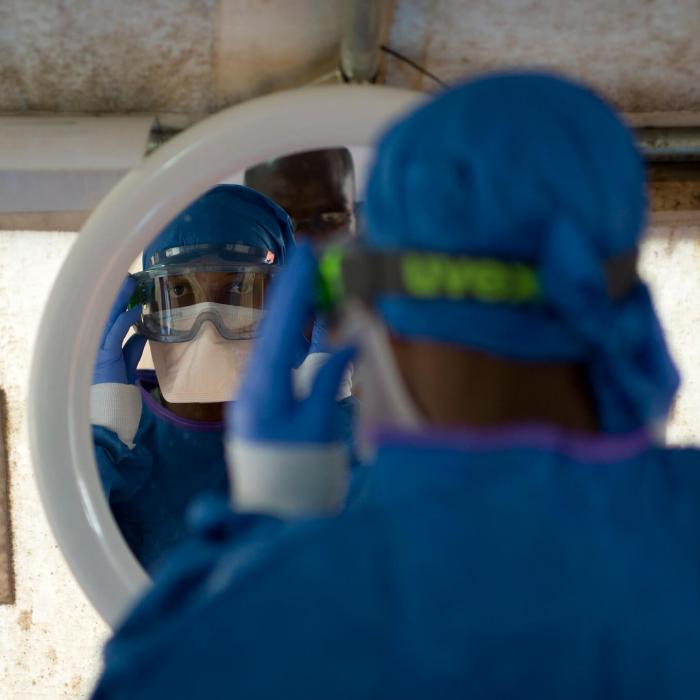
Responding to the coronavirus outbreak
Security for whom? Security from what?

And so it has happened. What many public health professionals and security experts had thought would eventually occur is now unfolding. It is perhaps what the World Health Organization (WHO) defines as a disease “X”, an unknown pathogen that causes human disease. A coronavirus pandemic is spreading across the world, including The Netherlands and most European countries. Pandemic outbreaks of viral and other pathogens are not new. They have been an integral part of human history but their travelling speed has increased by a factor of one hundred or more in the last century. To provide an idea about proportions: several influenza epidemics, including the Spanish flu (1918-1920), contributed to millions of deaths in the 20th century, leading to perhaps 20% of the world being infected. The most severe ongoing global pandemic is attributed to the HIV virus. More than 35 million people have died since the start of the epidemic in the 1980s; 37.9 million people are living with HIV/AIDS and around 1.7 million new HIV infections are diagnosed annually.
However, the novel coronavirus (its official name is COVID-19) is not similar to an influenza or HIV virus. This coronavirus is closely related biologically to the Severe Acute Respiratory Syndrome (SARS) that led to about 8,000 people being infected in 2003. The current coronavirus seems to be considerably more infectious than SARS and has already infected over 204,000 people globally. More than 8,200 people passed away.
Pandemic
Over the last few weeks, much has been written on the coronavirus outbreak. On 30 January 2020 the WHO declared the outbreak a public health emergency of international concern (PHEIC). Since 12th of March the global COVID-19 outbreak can be described as a pandemic. National public authorities and the WHO provide daily updates on the outbreak, including detailed advice on containment, prevention and public measures required. Many countries have installed aggressive public measures to contain the virus and more than 100 million Europeans are on lockdown. This scale is unprecedented. Several countries have started closing their borders, including some major economies. There are many reports about the impact the outbreak is having on global economic activities. Global financial markets have suffered heavy losses. Some argue that the vulnerability to trade and supply chain disruption indicates that economic globalisation has become too fragile and that there is a structural need to disintegrate and localise global production chains, including for meat and other food products. There is also much talk about security concerns, with countries like South Korea declaring a ‘war’ on the outbreak. The United States has declared a national emergency over the pandemic.
In this analysis we will outline some elements that have been relatively neglected by the media and the research community. These are: first, the individual human aspects of infection, disease and quarantine; second, the impact on health workers and healthcare systems; and third, the need for global cooperation and shared responsibilities to generate global public goods for health (GPGH).
Individual tragedies
Behind all those numbers of people who have been infected, passed away, survived or been subjected to quarantine are individual stories. These are real people, whether in China, Iran or Europe and with real feelings of fear, confusion and relief. While there has much been coverage of the death of Li Wenliang, the whistle-blower doctor who issued the first warnings about the outbreak, there is limited attention given to personal tragedies that have taken place. Liu Mengdi lost both her father and grandfather. A hospital in Iran was burned down by people due to coronavirus fears. A man in Italy had to wait 36 hours for authorities to collect his sister's body during the lockdown. She was buried without a funeral. Several countries have criminalised actions by people that potentially undermine containment and public health measures. There have been many xenophobic and racist incidents related to the coronavirus outbreak. Indeed, human rights considerations are quickly neglected and overruled, as shown by the lessons from the HIV epidemic. In the communication and panic generated through modern digital media we seem to believe that in a connected and globalised world we all carry a similar risk for infection. This is a false and flawed notion. Global health risks, potentials for crisis and related vulnerabilities are not evenly distributed. The Ebola outbreak indicated that these health risks follow structural injustices and neglect, and render invisible the people most affected by such global risks, such as the impoverished, the marginalised and the chronically ill.
Health systems
Effective and adequate public health responses to an epidemic rely on strong healthcare systems. However, in many places of the world healthcare systems are vulnerable and weak and can even become vector-sites for further infection. The Global Health Security index, the first comprehensive assessment and benchmarking of health security across 195 countries, concludes that most countries lack the fundamental healthcare capacity that is vital for responding to an epidemic. Not surprisingly, the weakest healthcare systems are found, with some exceptions, in low-income countries. Several of these countries already face the impacts of violent conflict, climate change and chronic malnutrition. Dr Tedros, Director General of the WHO, focused on these countries when the PHEIC was declared. ‘The main reason for this declaration is not because of what is happening in China, but because of what is happening in other countries. Our greatest concern is the potential for the virus to spread to countries with weaker health systems, and which are ill-prepared to deal with it.’ There has been much focus on the R&D investment required for a vaccine or medication against coronavirus. What is forgotten are the health workers who have to provide the medication and care for the patients. Health personnel have a disproportionate risk of contracting the virus. Over 3,000 healthcare workers were infected in China. Globally, there are shortages of personal protective equipment (PPE) such as masks, goggles and gloves. This might imply that in resource-limited settings healthcare workers will not be protected while treating coronavirus (suspected) patients. It is noteworthy to recall that there is a global shortage of around 18 million health workers, with 12 million needed in low-income countries. The coronavirus outbreak has created additional pressure on overstretched health systems, hospitals and primary healthcare teams that have been dealing with structural adjustment, austerity and underinvestment in the wake of the financial crisis of 2008-2009. This phenomenon takes place in European as well as African countries. An Italian nurse describes immense pressure and war-like conditions in the efforts to treat patients.
"If there is no health workforce, there is no global health security (GHS)."
If there is no health workforce, there is no global health security (GHS). For this reason, it is important to embed global health security efforts into programmes to attain Universal Health Coverage (UHC) and broader social protection strategies. In the word of Tedros, ‘GHS and UHC are two sides of the same coin.’
International Health Regulations and global public goods
The global governance of infectious disease control is conducted by the WHO and its International Health Regulations (IHR). These regulations were revised after the SARS outbreak in 2003. Through this legal framework, countries have agreed to build their capacities to detect, assess and report public health events. Moreover, it provides guidance on how to overcome unnecessary interference with international travel and trade. The problem is that many countries, including European, neglect and bypass the IHR. They do not neglect this in the narrow sense of the framework. Most countries notify the WHO of public health events that could have serious and international consequences. However, the broader solidarity principles of the IHR are ignored. This is the case for coronavirus and was also seen in relation to earlier PHEIC declarations, such as the Ebola outbreak in 2014-2015. Richer countries and other donors have not provided sufficient international financial assistance to other countries to meet the core public health capacitiesoutlined in the IHR (par.44). Only about a third of all 194 WHO member states have the core capacities in place to prepare for and respond to international public health threats.
"Only about a third of all 194 WHO member states have the core capacities in place to prepare for and respond to international public health threats."
The Global Health Security Agenda, a public-private partnership of 67 countries and other actors, aims to fill this technical and financial gap. Nevertheless, due to an erosion of the architecture of the international order, and specifically under pressure of the Trump administration, this initiative has not been as effective and sustainable as expected. Countries and donors have pledged US$289 million for the WHO coronavirus preparedness and response plan, for which US$675 million is needed. It must be noted that the WHO has already for a decade or so been financially in troubled waters due to political contestations between member states. In contrast, US$500 million worth of pandemic emergency financing (PEF) insurance bonds launched in 2017 by the World Bank received much criticism. The criteria to trigger payout is insanely complicated, with the terms relating to high-interest bonds heavily skewed towards private investors, while for the victims any payouts may come too late. Rather, experts advise that public funding for disease outbreak responses should be redirected through recognised mechanisms, such as the WHO contingency fund for emergencies. The preparedness for and response to international public health threats are global public goods. These must be financed and governed as such via the legitimate multilateral UN authority, the WHO, and for the Netherlands in close coordination with the other EU member states. Most likely, the coronavirus outbreak will trigger much debate about the need to reform the IHR specifically and infectious disease governance more generally.
A tipping point?
In summary, the coronavirus pandemic needs to be addressed seriously. Existing public health knowledge and measures are well able to deal with such an epidemic in an effective and proportionate way, thereby minimising the risks of social, economic and human disruption. There is, however, an absolute need for national governments to share responsibilities through financial and technical cooperation in order to protect people and to strengthen public health preparedness and response in countries and settings where there is more much risk of infection. Security for whom? Security from what? are essential questions to be asked in relation to this outbreak.
"Security for whom? Security from what? are essential questions to be asked in relation to this outbreak."
One could argue that a broader human security approach (‘freedom from fear, freedom from want’) might be the answer. The question is whether, and how, 25 years after the introduction of this concept by UNDP and given the ongoing ecological crisis, national governments are capable and willing to invest in this.
To conclude, Dutch sociologist Abram de Swaan wrote in a beautiful essay in 1998 on a Project for a Beneficial Epidemic, ‘…epidemics that are associated with poverty in other parts of the world may one day provoke concerted action by wealthy countries to eradicate the conditions of poverty that caused the spread of disease on a world scale’.Could this outbreak trigger such a cosmopolitan political momentum? The current trend of countries choosing national security concerns over international and human security matters indicates not. But who knows what will happen if the coronavirus pandemic lasts and the crisis becomes deep enough.
Acknowledgment to Simon Ruston for the title, as he wrote in 2011 ‘Global health security: Security for whom? Security from what?’
Follow @rvandepas and @clingendaelorg on Twitter